Annals of Antivirals and Antiretrovirals
Clinical presentation, ICU management and outcome in severe COVID-19 disease – A prospective observational study
Critical Care Medicine, Sir Gangaram Hospital, New Delhi, India
Author and article information
Cite this as
Shastri P (2023) Clinical presentation, ICU management and outcome in severe COVID-19 disease – A prospective observational study. Ann Antivir Antiretrovir. 2023; 7(1): 10-16. Available from: 10.17352/aaa.000017
Copyright License
© 2023 Shastri P. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.Aim: We conducted a prospective, observational study to describe the clinical characteristics, management, and outcomes of patients with moderate to severe coronavirus disease admitted to the Intensive Care Unit (ICU).
Methods: The study was conducted from 1st July 2020 to 31st December 2020. The criteria for ICU admission included a positive Reverse Transcriptase-Polymerase Chain Reaction (RT-PCR) for the novel Coronavirus (SARS-CoV-2) and oxygen saturation of less than 90% with or without oxygen.
Results: A total of 621 patients were included (median age, 59 years [interquartile range {IQR}, 48-68]; 75.8% were males. The common comorbidities were hypertension (323 [52%]), and diabetes mellitus. 96 (15.5%) patients underwent mechanical ventilation, 18 (2.9%) received renal replacement therapy, and 223 (36%) died. The median age in non-survivors was significantly higher [63 years (IQR 55-71)] vs. 57 years (IQR 46-66)] (p < 0.001). Hypoxia (oxygen saturation (SpO2 < 90%) and shortness of breath suggestive of impending respiratory failure were the most common symptoms necessitating ICU admission. A low absolute lymphocyte count (ALC), and high levels of inflammatory biomarkers which persisted for seven days after diagnosis were significantly associated with non-survival. Multivariate logistic regression analysis showed shortness of breath (SOB), hypoxia (SpO2 < 90% on oxygen), use of neuromuscular blockers, and chronic kidney disease as independent risk factors associated with mortality as were the severity scores (APACHE and SOFA).
Conclusion: This single-center case series provides clinical characteristics and outcomes of patients with confirmed COVID-19 disease admitted to the COVID ICU. These findings are important for guiding research and preparing for future pandemics.
The coronavirus infectious disease (COVID-19) has affected more than one billion people worldwide. It was declared a “public health emergency” by World Health Organization (WHO) in January 2020. In India, the first case was reported on 30 January 2020. A very strict lockdown was announced in the whole country on 25 March 2020. New cases reported per day peaked in mid-September (> 90,000 cases/day) and dropped to below 15,000 in January 2021 [1]. During this wave, the healthcare system was stretched, but multiple factors possibly contributed to the high mortality including delayed admission, old age, comorbidities and the lack of guidelines for uniform management [2].
The clinical features and the outcomes of these patients needs to be studied in details as it may vary in different populations. The virus is also known to mutate at periodic intervals. Studies on this group of patients have been described by authors from China [3], UK [4] and the United States [5]. These studies have indicated that increasing age and presence of co-morbidities are associated with increased mortality. Previous epidemiological studies on COVID-19 patients in India were mainly focussed on non-critical patients [2]. Peer-reviewed analysis of such patients in India has been limited. Additionally, quite a few studies were retrospective or had small sample size with inherent bias in study design.
The present study describes the demographics, comorbidities, clinical parameters, laboratory investigations, and outcomes of critically ill COVID-19 patients in a leading tertiary care centre in North India.
Methods
The study was conducted in a 650-bed tertiary care hospital from 1st July 2020 to 31st December 2020. After obtaining approval from the Institute Ethics Committee (EC/07/20/1697) and obtaining an informed consent either from the patient or their next of kin, all consecutive patients with a positive Reverse Transcriptase-Polymerase Chain Reaction (RT-PCR) from nasopharyngeal secretions, or endotracheal aspirate were enrolled as cases. The subjects were more than 18 years of age, and fulfilled the inclusion criteria as per the definition of a case of COVID-19 infection [6]. The criteria for ICU admission was a positive RT-PCR for novel Corona Virus (SARS-CoV-2) and oxygen saturation of less than 90% with or without oxygen. There were no formal exclusion criteria. The ICUs are closed adult units, and staffed by full-time intensive care physicians and nurses. The Case Report Form (CRF), was prepared after two rounds of pilot testing. The clinical data was collected prospectively from the patient’s charts and entered in a case report form. The data was subsequently transferred to a database in password protected computers. Demographic data including age, sex, contact information, date of admission and discharge, ICU scores on admission (APACHE II and SOFA) was collected. Hypoxia on admission was defined as a saturation (SpO2) of less than 90% with or without oxygen supplementation. The modality of oxygen therapy including decision to intubate was taken by the attending physician. We recorded the presence of comorbidities such as hypertension, coronary artery disease, chronic obstructive pulmonary disease, neurological disorder including stroke, chronic kidney disease, diabetes, organ transplant, malignancy and prior steroid therapy for auto immune conditions.
Complete Blood Count including absolute Lymphocyte Count (ALC), done on EFTA whole blood (Fluorescent based automated cell counter Sysmet CXN 1000). Renal and liver function tests were performed on Abbott alinity platform by end point spectrophotometry, and electrolytes by indirect ion specific electrodes., Inflammatory markers such as C Reactive Protein (CRP) by Nephelometry method, Ferritin and Interleukin-6 by Chemiluminescence microparticle immunoassay (CLIA), D-dimer (Quantitative Immuno-turbidimetric Assay, STA@ LIATEST D-D1), procalcitonin (Time resolved Adsorption cryptate TACE) was also recorded. Microbiological data was collected but not included in the analysis. Acute Kidney injury (AKI) was defined by KDIGO criteria [7] and Acute Respiratory Distress Syndrome (ARDS) as per Berlin definition [8].
The outcomes of all patients who completed their hospital course at the end of study (discharged alive or dead) were recorded. Primary outcome was hospital discharge or death. Secondary outcome measures included ICU mortality, and hospital length of stay (hospital-LOS). Additionally, COVID-19 management therapy data was also recorded to assess its possible effect on outcome.
Statistical analysis was performed using the statistical Package for Social Science (SPSS version 22, Chicago, IL, USA). The data for categorical variables were expressed as proportions and percentage (%) and continuous variables were expressed as mean ± standard deviation (SD) or the median and Interquartile Range (IQR). A Chi square or Fisher’s exact test (two-tailed) was used to compare categorical variables and unpaired Student’s t test to compare continuous variables. Microsoft Excel was used for constructing the graphs. Those parameters found significant (p < 0.05) were entered into a multivariate logistic regression analysis to identify independent risk factors associated with mortality; the results were presented as Odds Ratios (ORs) with 95% Confidence Intervals (CI) and p values. A p - value < 0.05 was considered statistically significant.
Results
We enrolled 621 patients admitted in the 60-bed dedicated ICU in the six-month period.
The median (IQR) age of the patients was 59 (48-68) years and 459 (74.8%) were males, the male-female ratio was 2.4:1. There were 37 (5.9 %) health care workers in the cohort. Only, two patients had travel history. Obesity (BMI > 25 kg/m2) was present in 21(3.4%) of cases.
The age group of 50-70 years was the most affected (423, 68.1%) and this cohort had a crude mortality of 23.8%.
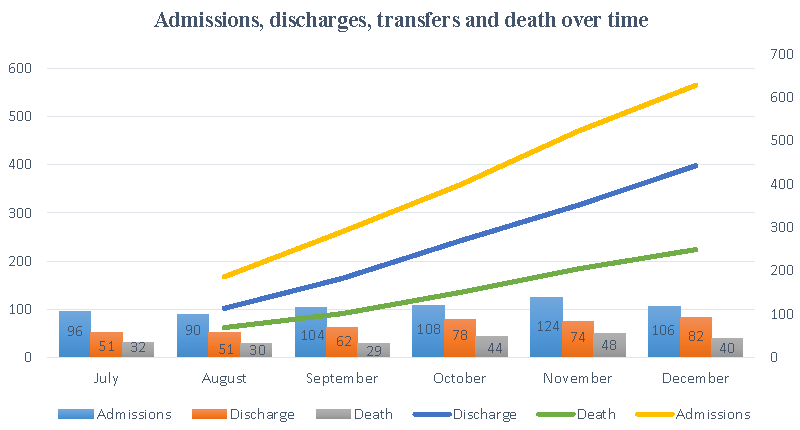
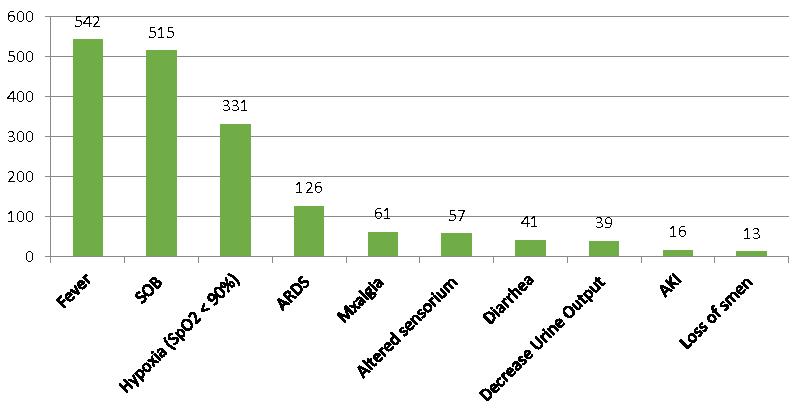
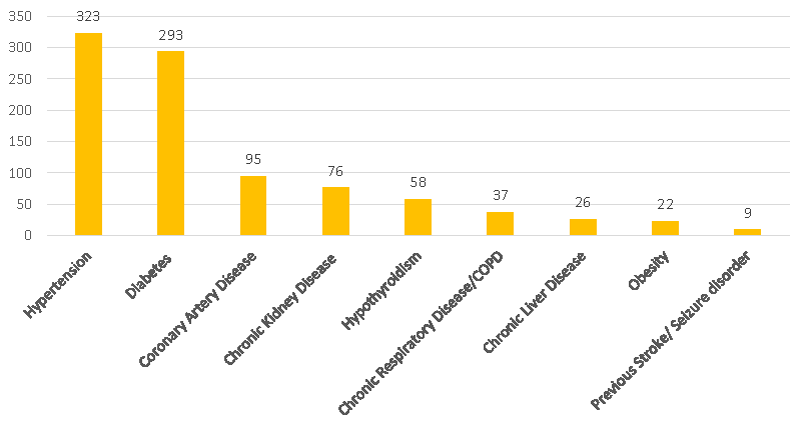
The number of admissions, discharges, and deaths over time are shown in Figure 1. The age and sex distribution, severity scores and outcomes of the entire cohort is shown in Tables 1. A significant number of patients presented with organ dysfunction to ICU as depicted by the severity scores. Presenting symptoms in order of frequency is shown in Figure 2. The most common comorbidities were hypertension (323 [52%]), and type 2 diabetes mellitus [294 (47.2%)] (Figure 3).
Acute Kidney Injury (AKI) and Acute Respiratory Distress Syndrome (ARDS) were present in 18 (2.9%) and 128 (20.3%) of cases respectively. 305 (49.11%) number of patients were treated with Non-Invasive Ventilation (NIV) or High Frequency Nasal Canulae (HFNC); 96 (15.5%) received invasive mechanical ventilation (23 survived), 15 (4.03%) patients underwent tracheostomy. 34 (35.4%) of intubated patients underwent prone ventilation (9 survived) and 10 (3.9%) patients underwent extracorporeal membrane oxygenation (ECMO) (none survived).
Majority of patients [584 (92.9%)] received prophylactic antibiotics and Deep Vein Thrombosis (DVT) prophylaxis. The most preferred antibiotics was betalactam-betalactam inhibitor (BL-BLI) in combination with macrolides, and enoxaparin was the preferred agent for DVT prophylaxis. Majority of patients (588, 94.7%) patients received steroids, 355 (57.2%) survived. Dexamethasone was the drug most commonly used.
The case fatality was 36% in the entire cohort. The total hospital admission in the study time period was 32575 producing a burden of 19.09 COVID patients/1000 hospital admissions.
To assess the risk factors, we divided the cohort into two groups: survivors and non survivors.
There was a significant difference observed in the median age of survivors [57 (IQR 46-66)] years as compared to non-survivors [63(IQR 55-71)] years (p < 0.001). Among clinical symptoms hypoxia on admission [179 (79.9%) vs. 152(38.3%)] was significantly higher among non survivors Table 2, (Figure 2). Among patients who developed ARDS again the incidence was significantly higher in non-survivors [99 (44.2% vs. 27 (6.8%), p < 0.001]
In the laboratory parameters a low absolute lymphocyte count (ALC) was significantly associated with non-survival (906 ± 1070 in non survivors vs. 1145 ± 1075 in survivors p = <0.001). This persisted on day 7 when the mean ALC Count was 471(320±800) in non-survivor’s vs. 1059 (689±1586) in survivors (p < 0.001). A likely cause of lymphopenia could be direct viral invasion and lysis as lymphocytes express the ACE2 receptor on their surface. Laboratory investigations for organ dysfunction (renal, hepatic, coagulation) were significantly abnormal among non-survivors as compared to survivors (Table 3).
Among the comorbidities chronic kidney disease (CKD), chronic liver disease (CLD), hypertension and type 2 diabetes mellitus were statistically significant in non-survivors. The use of Convalescent plasma, Neuro muscular blockers (NMB) and monoclonal antibodies were given in relatively few cases. Antivirals (mainly remdesvir), anticoagulants (mainly Enoxaparin) and steroids were administered in a majority of cases. Dexamethasone was the most common steroid given in 355 (89.2%) survivors and 213 (95.1%) of non-survivors, a difference which was statistically significant (p = 0.012). Among 96 patients who underwent mechanical ventilation 23(5.8%) survived as compared to 73 (32.67%) who did not (p < 0.001). Tracheostomy was done in 24 patients equally divided among survivors and non-survivors. The levels of inflammatory biomarkers, (CRP, Ferritin, IL-6, and D-dimer) were twice that in non-survivors as compared to survivors and continued to be significantly higher on day 7 (Figure 4). At 28 days 37 of the surviving patients were still hospitalised with 5 patients on NIV and one on invasive ventilation (Table 4). Variables which were found to be significant (p < 0.05) in the univariate logistic analysis were included in multivariate logistic regression. Those independently associated with the risk of mortality included shortness of breath (SOB) OR 1.9 (CI 1.01-3.62), Hypoxia OR 2.0 (95% CI 1.02-3.33), ARDS OR 4.83 (CI 2.68-8.71), chronic kidney disease OR 1.97 (CI 1.06-3.68). Use of neuromuscular blockers OR 0.228 CI 0.113-0.461, the severity scores SOFA OR 0.83(CI 0.7-0.9) and APACHE OR 0.86 (CI 0.8-0.9) were also independently associated with mortality (Table 5).
Discussion
To the best of our knowledge, this is the largest prospective cohort of patients with COVID-19 in a dedicated COVID ICU from India. A total of 621 confirmed cases of COVID-19 were enrolled and followed till death or hospital discharge. The median (IQR) age of the patients was 59 (48-68) years with a case fatality of 36%. Compared to other studies a relatively younger population was affected while it is known that elderly patients with comorbidities had the highest risk of death in previous studies [3,5]. Among clinical symptoms, shortness of breath, and hypoxia suggestive of respiratory failure were the most common presentation in non-survivors, indicating the association of these parameters with COVID-19 severity and poor outcome [3].
Lymphopenia and its persistence rather than reversal was a significant finding among non-survivors in our study, similar conclusion has been reported in a meta-analysis [9]. Many studies including a meta-analysis have demonstrated that a high Neutrophil to Lymphocyte Ratio (NLR) as an independent risk factor for severe disease serving as an early warning sign. A high NLR implies a dysfunctional response, with increased neutrophils and decreased lymphocytes [10].
In the present study hypertension, the most common comorbidity was associated with a mortality of 20.7%. Patients with pre-existing Coronary Artery Disease (CAD) had a mortality of 6.4%. The prevalence of hypertension and CAD was approximately 21.1% and 8.4%, respectively in a meta-analysis of 1576 patients with COVID-19 indicating that patients with cardiovascular disease accounts for a large proportion of COVID-19 deaths [11]. Hypertension besides age> 50 years and male sex has been included in a risk score to identify patients at risk of developing severe disease [12]. The virus uses the Angiotensin Converting Enzyme receptor (ACE2) to enter into cells. Angiotensin Receptor Blockers (ARB) and ACE inhibitors, increase ACE2 mRNA expression. It has been hypothesized that COVID-19 patients who are on Renin Angiotensin Aldasterone (RAAS) inhibitors may develop more serious disease [13]. However, the evidence in favour of this hypothesis is conflicting [14-16].
Diabetes was the second most common comorbidity (294, 47.2%) in which the mortality was 19%. This is considerably higher than that in published literature [17-19] probably because we included patients from ICU with severe disease as indicated by the relatively higher APACHE Score. Diabetes predisposes the patients to have severe disease, as shown in a Chinese study which reported a higher prevalence of diabetes among patients with severe COVID-19 (16.2% vs. 5.7%) as compared to patients with non-severe disease [20]. The US Centre for Disease Control and Prevention reported that the prevalence of diabetes was 32.4% in ICU patients as compared to 24.2% in patients admitted to wards [21].
We could not assess the impact of outcome on obesity because of small number of patients in the study, but it is recognized as a significant risk factor for increased mortality [4].
The inflammatory biomarkers are usually increased during the cytokine storm or during acute phase of the disease. The serum biomarkers levels including CRP, LDH, Ferritin, IL-6, and D-dimer were consistently higher even on day 7 after admission in non-survivors and correlated with the severity of the disease (Figure 4). Several studies and at least one meta-analyses have reported similar findings regarding their association with poor outcome [22,23]. C-reactive protein is significantly correlated with ferritin and IL-6 and suggestive of elevated inflammatory response in COVID-19. In an Indian study [24] the mean CRP was significantly increased in severe cases and a cut-off value > 48 mg/dl was proposed to indicate an increased risk of mortality. Besides, Wang, et al. [25] showed that AST, ALT, LDH, and D-dimer levels were significantly increased in critical COVID-19 patients. High IL-6 correlated with severity, and bilateral lung involvement [26]. A meta-analysis found IL-6 as an important marker of disease severity and predictor of mortality, besides being effective in monitoring the response [27].
Abnormal coagulation in COVID-19 is characterized by a high fibrinogen, prothrombin time and activated partial thromboplastin time are normal or mildly prolonged, thrombocytopenia is mild (platelet count > 100 × 103/ml), spontaneous bleeding is rare [28]. Several meta-analyses have shown that D-dimer levels have prognostic value and correlate with disease severity and in-hospital mortality. Moreover, they can be used to guide clinical management. A level of > 2.0μg/ml on admission could predict mortality [29,30].
The management strategy against COVID-19 was not uniform during the first wave. Multiple therapeutic options including antiviral drugs (remdesivir), convalescent plasma, anti-inflammatory drugs, steroids (dexamethasone) and immunomodulators were used globally [31]. In the present study the use Convalescent plasma and NM blocker were associated with non-survival but maybe they were given in the sicker patients indicating selection bias. The proportion of patients receiving remdesvir was similar in survivors (61.6%) and non-survivors (55.4%) Monoclonal antibiotics were given to very few patients (26, 4.2%). The use of steroids was associated with non-survival, 355(89.2%) of survivors, and 213(95.1%) of non-survivors received steroids. This was unlike the Recovery trial which showed decreased mortality in the patients receiving dexamethasone as compared to the control group in mechanically ventilated patients [32].
NIV and HFNC was utilized in 49% of cases. According to a meta-analysis [33], its utility in hypoxic COVID-19 adult patients remains uncertain, but it been shown to be an effective in reducing mortality and preventing intubation. The meta-analysis recommended its use in COVID-19 patients in centres where close monitoring and experienced staff is present [34]. Concern has been expressed that they may delay tracheal intubation and exacerbate self-inflicted lung injury [7].
Multivariate analysis showed that only shortness of breath. hypoxia, use of NM blockers, ARDS, and CKD were independent predictors of mortality. The limitation of the study was that, the detailed data on ventilatory settings was not recorded, except that a greater proportion of ventilated patients died. Therefore, our finding that hypoxia, ARDS and mortality being related should be taken with caution.
Again, we did not look into prior drug therapy (such as prior use of angiotensin converting enzyme inhibitors) in hypertensive patients and its impact on the outcome. Invasive mechanical ventilation settings, cut offs of inflammatory biomarkers and their association with clinical outcomes in COVID-19 patients can be a subject for future research. Another limitation is that, though a majority of patients required organ support we did not analyse the association of vasopressor use, or renal replacement therapy in the present study. Strengths of our study include its relatively large sample size, complete recording of data of patients admitted to the dedicated ICU, the prospective design using a standardised case reporting form, and follow-up until patient discharge or death in every patient.
SARS-CoV-2 will continue to remain with us, albeit with new variants, which can escape the vaccines. There is an urgent need to provide guidance for specific geographical regions with readily accessible tools to tailor clinical decision-making in COVID-19 patients. COVID-19 highlighted the strengths, and weaknesses of our health care system. Studies of this kind depicting the magnitude of the problem will help decision makers in creating ICU and hospital capacity, including laboratories and developing new clinical protocols. With the pandemic dying down, researchers are able to communicate more effectively, a rational approach to achieve this can be expected.
Conclusion
This study describes the clinical characteristics and outcomes of patients with COVID-19 in ICU patients in India. COVID-19 affected people in the age group of 50-70 years, predominantly males. The clinical manifestation, suggesting impending respiratory failure can predict the outcome in critically ill of patients. ICU severity scores (SOFA and APACHE) and the laboratory parameters indicating organ dysfunction can help in triage of these patients. Steroids in this study was not associated with greater survival, though it was not independently associated with mortality. No other specific therapy can be recommended. Supportive therapy including strict infection control measures remain the cornerstone in the management of patients with COVID-19 disease. Further understanding of the pathogenesis and the role of supportive management therapy is needed.
Funding
No cost was borne by patients or investigators for this study. The drugs were available via the hospital supply.
Ethical clearance
Institutional ethical committee clearance was obtained prior to study.
We gratefully acknowledge the contribution of Mr DK Shukla for his contribution towards data analysis.
- Sarkar A, Chakrabarti AK, Dutta S. Covid-19 Infection in India: A Comparative Analysis of the Second Wave with the First Wave. Pathogens. 2021 Sep 21;10(9):1222. doi: 10.3390/pathogens10091222. PMID: 34578254; PMCID: PMC8469101.
- Bobdey S, Chawla N, Behera V, Ray S, Ilankumaran M, Koshy G, Kaushik SK. An analysis of mortality and survival of COVID 19 patients admitted to a tertiary care hospital in Maharashtra, India. Med J Armed Forces India. 2021 Jul;77(Suppl 2):S353-S358. doi: 10.1016/j.mjafi.2021.02.004. Epub 2021 Jul 26. PMID: 34334904; PMCID: PMC8313027.
- Yang X, Yu Y, Xu J, Shu H, Xia J, Liu H, Wu Y, Zhang L, Yu Z, Fang M, Yu T, Wang Y, Pan S, Zou X, Yuan S, Shang Y. Clinical course and outcomes of critically ill patients with SARS-CoV-2 pneumonia in Wuhan, China: a single-centered, retrospective, observational study. Lancet Respir Med. 2020 May;8(5):475-481. doi: 10.1016/S2213-2600(20)30079-5. Epub 2020 Feb 24. Erratum in: Lancet Respir Med. 2020 Apr;8(4):e26. PMID: 32105632; PMCID: PMC7102538.
- Thomson RJ, Hunter J, Dutton J, Schneider J, Khosravi M, Casement A, Dhadwal K, Martin D. Clinical characteristics and outcomes of critically ill patients with COVID-19 admitted to an intensive care unit in London: A prospective observational cohort study. PLoS One. 2020 Dec 15;15(12):e0243710. doi: 10.1371/journal.pone.0243710. PMID: 33320904; PMCID: PMC7737956.
- Cummings MJ, Baldwin MR, Abrams D, Jacobson SD, Meyer BJ, Balough EM, Aaron JG, Claassen J, Rabbani LE, Hastie J, Hochman BR, Salazar-Schicchi J, Yip NH, Brodie D, O'Donnell MR. Epidemiology, clinical course, and outcomes of critically ill adults with COVID-19 in New York City: a prospective cohort study. Lancet. 2020 Jun 6;395(10239):1763-1770. doi: 10.1016/S0140-6736(20)31189-2. Epub 2020 May 19. PMID: 32442528; PMCID: PMC7237188.
- WHO. WHO COVID-19 Case definition. updated in Public health surveillance for COVID-19 https://www.who.int/publications/i/item/WHO-2019-nCoV-11.
- Khwaja A. KDIGO clinical practice guidelines for acute kidney injury. Nephron Clin Pract. 2012;120(4):c179-84. doi: 10.1159/000339789. Epub 2012 Aug 7. PMID: 22890468.
- Singer M, Deutschman CS, Seymour CW, Shankar-Hari M, Annane D, Bauer M, Bellomo R, Bernard GR, Chiche JD, Coopersmith CM, Hotchkiss RS, Levy MM, Marshall JC, Martin GS, Opal SM, Rubenfeld GD, van der Poll T, Vincent JL, Angus DC. The Third International Consensus Definitions for Sepsis and Septic Shock (Sepsis-3). JAMA. 2016 Feb 23;315(8):801-10. doi: 10.1001/jama.2016.0287. PMID: 26903338; PMCID: PMC4968574.
- Huang I, Pranata R. Lymphopenia in severe coronavirus disease-2019 (COVID-19): systematic review and meta-analysis. J Intensive Care. 2020 May 24;8:36. doi: 10.1186/s40560-020-00453-4. PMID: 32483488; PMCID: PMC7245646.
- Lagunas-Rangel FA. Neutrophil-to-lymphocyte ratio and lymphocyte-to-C-reactive protein ratio in patients with severe coronavirus disease 2019 (COVID-19): A meta-analysis. J Med Virol. 2020 Oct;92(10):1733-1734. doi: 10.1002/jmv.25819. Epub 2020 Apr 8. PMID: 32242950; PMCID: PMC7228336.
- Yang J, Zheng Y, Gou X, Pu K, Chen Z, Guo Q, Ji R, Wang H, Wang Y, Zhou Y. Prevalence of comorbidities and its effects in patients infected with SARS-CoV-2: a systematic review and meta-analysis. Int J Infect Dis. 2020 May;94:91-95. doi: 10.1016/j.ijid.2020.03.017. Epub 2020 Mar 12. PMID: 32173574; PMCID: PMC7194638.
- Shi Y, Yu X, Zhao H, Wang H, Zhao R, Sheng J. Host susceptibility to severe COVID-19 and establishment of a host risk score: findings of 487 cases outside Wuhan. Crit Care. 2020 Mar 18;24(1):108. doi: 10.1186/s13054-020-2833-7. PMID: 32188484; PMCID: PMC7081524.
- Fang L, Karakiulakis G, Roth M. Are patients with hypertension and diabetes mellitus at increased risk for COVID-19 infection? Lancet Respir Med. 2020 Apr;8(4):e21. doi: 10.1016/S2213-2600(20)30116-8. Epub 2020 Mar 11. Erratum in: Lancet Respir Med. 2020 Jun;8(6):e54. PMID: 32171062; PMCID: PMC7118626.
- Vaduganathan M, Vardeny O, Michel T, McMurray JJV, Pfeffer MA, Solomon SD. Renin-Angiotensin-Aldosterone System Inhibitors in Patients with Covid-19. N Engl J Med. 2020 Apr 23;382(17):1653-1659. doi: 10.1056/NEJMsr2005760. Epub 2020 Mar 30. PMID: 32227760; PMCID: PMC7121452.
- Meng J, Xiao G, Zhang J, He X, Ou M, Bi J, Yang R, Di W, Wang Z, Li Z, Gao H, Liu L, Zhang G. Renin-angiotensin system inhibitors improve the clinical outcomes of COVID-19 patients with hypertension. Emerg Microbes Infect. 2020 Dec;9(1):757-760. doi: 10.1080/22221751.2020.1746200. PMID: 32228222; PMCID: PMC7170368.
- Kuba K, Imai Y, Rao S, Gao H, Guo F, Guan B, Huan Y, Yang P, Zhang Y, Deng W, Bao L, Zhang B, Liu G, Wang Z, Chappell M, Liu Y, Zheng D, Leibbrandt A, Wada T, Slutsky AS, Liu D, Qin C, Jiang C, Penninger JM. A crucial role of angiotensin converting enzyme 2 (ACE2) in SARS coronavirus-induced lung injury. Nat Med. 2005 Aug;11(8):875-9. doi: 10.1038/nm1267. Epub 2005 Jul 10. PMID: 16007097; PMCID: PMC7095783.
- Ejaz H, Alsrhani A, Zafar A, Javed H, Junaid K, Abdalla AE, Abosalif KOA, Ahmed Z, Younas S. COVID-19 and comorbidities: Deleterious impact on infected patients. J Infect Public Health. 2020 Dec;13(12):1833-1839. doi: 10.1016/j.jiph.2020.07.014. Epub 2020 Aug 4. PMID: 32788073; PMCID: PMC7402107.
- Ng WH, Tipih T, Makoah NA, Vermeulen JG, Goedhals D, Sempa JB, Burt FJ, Taylor A, Mahalingam S. Comorbidities in SARS-CoV-2 Patients: a Systematic Review and Meta-Analysis. mBio. 2021 Feb 9;12(1):e03647-20. doi: 10.1128/mBio.03647-20. PMID: 33563817; PMCID: PMC7885108.
- Richardson S, Hirsch JS, Narasimhan M, Crawford JM, McGinn T, Davidson KW; the Northwell COVID-19 Research Consortium; Barnaby DP, Becker LB, Chelico JD, Cohen SL, Cookingham J, Coppa K, Diefenbach MA, Dominello AJ, Duer-Hefele J, Falzon L, Gitlin J, Hajizadeh N, Harvin TG, Hirschwerk DA, Kim EJ, Kozel ZM, Marrast LM, Mogavero JN, Osorio GA, Qiu M, Zanos TP. Presenting Characteristics, Comorbidities, and Outcomes Among 5700 Patients Hospitalized With COVID-19 in the New York City Area. JAMA. 2020 May 26;323(20):2052-2059. doi: 10.1001/jama.2020.6775. Erratum in: JAMA. 2020 May 26;323(20):2098. PMID: 32320003; PMCID: PMC7177629.
- Guan WJ, Ni ZY, Hu Y, Liang WH, Ou CQ, He JX, Liu L, Shan H, Lei CL, Hui DSC, Du B, Li LJ, Zeng G, Yuen KY, Chen RC, Tang CL, Wang T, Chen PY, Xiang J, Li SY, Wang JL, Liang ZJ, Peng YX, Wei L, Liu Y, Hu YH, Peng P, Wang JM, Liu JY, Chen Z, Li G, Zheng ZJ, Qiu SQ, Luo J, Ye CJ, Zhu SY, Zhong NS; China Medical Treatment Expert Group for Covid-19. Clinical Characteristics of Coronavirus Disease 2019 in China. N Engl J Med. 2020 Apr 30;382(18):1708-1720. doi: 10.1056/NEJMoa2002032. Epub 2020 Feb 28. PMID: 32109013; PMCID: PMC7092819.
- CDC COVID-19 Response Team. Preliminary Estimates of the Prevalence of Selected Underlying Health Conditions Among Patients with Coronavirus Disease 2019 - United States, February 12-March 28, 2020. MMWR Morb Mortal Wkly Rep. 2020 Apr 3;69(13):382-386. doi: 10.15585/mmwr.mm6913e2. PMID: 32240123; PMCID: PMC7119513.
- Kadhim AS, Abdullah YJ. Serum levels of interleukin-6, ferritin, C-reactive protein, lactate dehydrogenase, D-dimer, and count of lymphocytes and neutrophils in COVID-19 patients: Its correlation to the disease severity. Biomed Biotechnol Res J. 2021; 5:69-73 doi: 10.4103/bbrj.bbrj_188_20
- Huang I, Pranata R, Lim MA, Oehadian A, Alisjahbana B. C-reactive protein, procalcitonin, D-dimer, and ferritin in severe coronavirus disease-2019: a meta-analysis. Ther Adv Respir Dis. 2020 Jan-Dec;14:1753466620937175. doi: 10.1177/1753466620937175. PMID: 32615866; PMCID: PMC7336828.
- Sakthivadivel V, Bohra GK, Maithilikarpagaselvi N, Khichar S, Meena M, Palanisamy N, Gaur A, Garg MK. Association of Inflammatory Markers with COVID-19 Outcome among Hospitalized Patients: Experience from a Tertiary Healthcare Center in Western India. Maedica (Bucur). 2021 Dec;16(4):620-627. doi: 10.26574/maedica.2021.16.4.620. PMID: 35261664; PMCID: PMC8897805.
- Wang D, Li R, Wang J, Jiang Q, Gao C, Yang J, Ge L, Hu Q. Correlation analysis between disease severity and clinical and biochemical characteristics of 143 cases of COVID-19 in Wuhan, China: a descriptive study. BMC Infect Dis. 2020 Jul 16;20(1):519. doi: 10.1186/s12879-020-05242-w. PMID: 32677918; PMCID: PMC7364396.
- Liu T, Zhang J, Yang Y, Ma H, Li Z, Zhang J, Cheng J, Zhang X, Zhao Y, Xia Z, Zhang L, Wu G, Yi J. The role of interleukin-6 in monitoring severe case of coronavirus disease 2019. EMBO Mol Med. 2020 Jul 7;12(7):e12421. doi: 10.15252/emmm.202012421. Epub 2020 Jun 5. PMID: 32428990; PMCID: PMC7280589.
- Zeng F, Huang Y, Guo Y, Yin M, Chen X, Xiao L, Deng G. Association of inflammatory markers with the severity of COVID-19: A meta-analysis. Int J Infect Dis. 2020 Jul;96:467-474. doi: 10.1016/j.ijid.2020.05.055. Epub 2020 May 18. PMID: 32425643; PMCID: PMC7233226.
- Mitchell WB. Thromboinflammation in COVID-19 acute lung injury. Paediatr Respir Rev. 2020 Sep;35:20-24. doi: 10.1016/j.prrv.2020.06.004. Epub 2020 Jun 11. PMID: 32653469; PMCID: PMC7289106.
- Zhang L, Yan X, Fan Q, Liu H, Liu X, Liu Z, Zhang Z. D-dimer levels on admission to predict in-hospital mortality in patients with Covid-19. J Thromb Haemost. 2020 Jun;18(6):1324-1329. doi: 10.1111/jth.14859. PMID: 32306492; PMCID: PMC7264730.
- Yao Y, Cao J, Wang Q, Shi Q, Liu K, Luo Z, Chen X, Chen S, Yu K, Huang Z, Hu B. D-dimer as a biomarker for disease severity and mortality in COVID-19 patients: a case control study. J Intensive Care. 2020 Jul 10;8:49. doi: 10.1186/s40560-020-00466-z. PMID: 32665858; PMCID: PMC7348129.
- Welte T, Ambrose LJ, Sibbring GC, Sheikh S, Müllerová H, Sabir I. Current evidence for COVID-19 therapies: a systematic literature review. Eur Respir Rev. 2021 Mar 17;30(159):200384. doi: 10.1183/16000617.0384-2020. PMID: 33731328; PMCID: PMC9489065.
- RECOVERY Collaborative Group; Horby P, Lim WS, Emberson JR, Mafham M, Bell JL, Linsell L, Staplin N, Brightling C, Ustianowski A, Elmahi E, Prudon B, Green C, Felton T, Chadwick D, Rege K, Fegan C, Chappell LC, Faust SN, Jaki T, Jeffery K, Montgomery A, Rowan K, Juszczak E, Baillie JK, Haynes R, Landray MJ. Dexamethasone in Hospitalized Patients with Covid-19. N Engl J Med. 2021 Feb 25;384(8):693-704. doi: 10.1056/NEJMoa2021436. Epub 2020 Jul 17. PMID: 32678530; PMCID: PMC7383595.
- Shallik N, Bashir K, Elmoheen A, Iftikhar H, Zaki HA. High flow nasal oxygen (HFNO) in the treatment of COVID-19 infection of adult patients from – An emergency perspective: A systematic review and meta-analysis. Trends in Anaesthesia & Critical Care. 2023 ;50:101238. doi: 10.1016/j.tacc.2023.101238.
- Meng L, Qiu H, Wan L, Ai Y, Xue Z, Guo Q, Deshpande R, Zhang L, Meng J, Tong C, Liu H, Xiong L. Intubation and Ventilation amid the COVID-19 Outbreak: Wuhan's Experience. Anesthesiology. 2020 Jun;132(6):1317-1332. doi: 10.1097/ALN.0000000000003296. PMID: 32195705; PMCID: PMC7155908.
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.


 Save to Mendeley
Save to Mendeley
